MRCO BLOG
Medical Musings, Health Hypotheses & Therapeutic Thoughts
|
Dr. Edmund Bruce-Gardner Some not so good news... For years (about eighty or so!) the general medical consensus has been that FSS has a ‘self-limiting natural history’, a progression that will – frustratingly slowly, but inexorably – grind its way through to full recovery, even with no treatment. However, a recently published review [i] suggests that “[n]o evidence supported the theory of progression through recovery phases to full resolution without treatment”. Basically, the upshot is, if you have a frozen shoulder, you should probably have it looked at! But what to do…? As you may have guessed, with little consensus on the causes of frozen shoulder, there is a generously large range of treatment options, both conservative and surgical. Essentially, all of the following are attempting to either: (a) decrease pain (b) improve shoulder function (c) improve shoulder range of movement (RoM) (d) all of the above Osteopathic Treatment 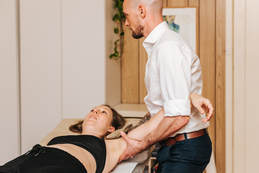 Osteopathic treatment for frozen shoulder is aimed at getting through each of the above stages as quickly as possible. Depending on the progression of the condition, treatment will have slightly different aims. We use techniques such as articulation (controlled movement) of the shoulder complex to help maintain as much movement as possible – and this needs to be directed not just to the glenohumeral joint – or shoulder proper – but the other articulations we talked about in our initial post on the shoulder. The scapulothoracic articulation (which is not a true joint at all, but the way that we think about how the shoulder blade interacts with the rest of the back and ribs) is often crucial in this. Soft-tissue techniques, aimed at the muscles, tendons and ligaments, can also help maintain range of movement and reduce pain levels. Acupuncture/dry needling can be helpful as an adjunct to this, although there is a lack of good-quality evidence to back this up. Also as mentioned in our first shoulder post, the neck and jaw are also closely related to the shoulder, as well as the thoracic spine (mid-back) and ribs. It is nearly always a good idea to look at the other shoulder as well. Assessment and treatment of all of these can help to reduce the pain by removing barriers to good function – you can think of it as your body trying to juggle too many balls, and not particularly well. By removing some of the other balls, you can focus on the ones that are left more effectively. An osteopathic approach to FSS will also rely heavily on:  Exercise One thing we do know is that further immobility carries the risk of creating a vicious spiral, where pain and restriction leads the patient to avoid using the arm, which makes it stiffer (and, in the freezing phase, sorer as well), which leads to decreased use… So, it makes sense to keep using the arm as much as possible within pain-free range. Those of you who have seen me in my professional capacity can skip this bit, because you’ve heard it (many times) before…! It is important to note that there is (in my view) a big difference between pain and discomfort. Pain is a warning signal, and will cause your body to try and protect itself any way it knows how – which is a depressingly short list, headed up by tightening every muscle it can to try and protect the area and prevent more damaging (as far as the body is concerned) movement. Discomfort is more of an early-warning system than a panic button, and allows us to tell when we are approaching an area that our body wants us to be careful of. Discomfort is pretty unavoidable when you have ‘pissed-off body parts’, and we are not concerned with it. Pain, on the other hand, has no place at the clinic, or in our lives. Anyway, where was I…? So, exercises designed to prevent decrease (during freezing) or increase range of movement (in frozen and thawing phases) should be done within the limits and tolerances of pain – indeed, there is evidence to suggest that these will increase mobility more than aggressive stretching[ii],[iii]. Medication (oral) Both NSAIDs (non-steroidal anti-inflammatories) and steroids can reduce pain and therefore help increase range of movement, but the positive effects are generally rather short-term. Steroids are rarely used due to the potential for adverse effects and the limited nature of their relief. NSAIDs also have problems if taken long-term, particularly if you have existing gut issues or other conditions. Intra-articular infiltration This is the technical-speak for a medication (steroid) injection inside the painful shoulder. Again, relief is limited (often no longer than six weeks), and tends to be most effective if given early in the progression of the condition. Other non-surgical interventions There are a number of other interventions that are used, primarily to help combat the pain and relax the muscles and possibly capsule around the shoulder. Low-level laser therapy can be used for pain relief, as well as improving shoulder function, but a 2013 systematic review suggests it is not very helpful for improving RoM[iv]. TENS (transcutaneous electrical nerve stimulation) is a way of using electrical currents to ‘trick’ the body into feeling less pain, and can be useful for short-term pain relief. If you find TENS helpful, I would strongly recommend getting your own unit and using it at home, rather than going to someone for treatment. Heat applied locally can also help with pain and muscle tension. Again, it will give no lasting relief, but can help manage the symptoms. Ultrasound is another commonly-used modality, but the same systematic review mentioned above found it unhelpful for pain relief or improvement of function or RoM xv. However, remember that the body does not read textbooks or research papers, so it is often worth exploring all available options.. Your body may respond fantastically to [x] intervention; all research does is play the numbers so we can say “in most cases, this does/doesn’t work”. Mobilisation under anaesthetic (MUA) To be honest, this one is pretty barbaric. They basically knock you out with anaesthetic, then, free from pesky considerations like the patient screaming like a rampaging elephant, rip the arm around to free up the restrictions or contractures. To illustrate how much force this involves, consider that the surgeon has to be careful to hold high up the arm (near the shoulder) to ‘minimise’ the risk of your arm breaking instead. There is also the fact that in at least one randomized controlled trial, no difference was found between those who underwent an MUA followed by a home exercise program, versus those who completed a home exercise program alone[v]. Arthroscopic capsular release This is a more sophisticated version of MUA. It is a version of keyhole surgery, using a little camera. The surgeon can see which parts of the capsule are involved, and target them specifically, rather than just ripping the arm upwards and into various degrees of rotation. This type of intervention may be worthy of consideration if e.g. you have a rotator cuff tear that is thought to be contributing to your issues, and the surgeon can effect the repair at the same time. Hydrodilatation (or capsular distension) This basically involves injecting fluid into the shoulder capsule to help stretch (or distend) it. It might involve injecting saline (salt water), air, or contrast fluid. Corticosteroids (to reduce inflammation) or anaesthetic (to reduce pain) may also be included. Hydrodilatation seems to give good short-term results for improved RoM, shoulder function, and pain reduction, and so may be helpful in patients for whom osteopathy/physiotherapy/etc and other non-surgical interventions have not been helpful. Speaking purely anecdotally, I have had several patients who have not responded to cortisone (steroid) injections, but hydrodilatation plus steroids seemed to do the trick. .... So, all in all, considering how common – and how potentially debilitating – frozen shoulder can be, we don’t know enough about why it happens or the relative value of the various interventions to tell you unequivovally what you can do about it. However, there are a few things we do know. One is that despite the received wisdom of the last eighty or so years, FSS does not appear to be a self-limiting condition; that is, it may go away if you wait long enough, but it probably will not. So, seeking some form of assessment and treatment for your (possible) frozen shoulder is probably a good idea. I think it also makes sense to start with the least invasive and potentially uncomfortable interventions, or those with the least risk of side-effects (like broken bones, cartilage damage etc.). The other is the role of immobilisation in the development of frozen shoulder. Given that, early mobilisation of the shoulder after any trauma or surgery (whether to the shoulder or not) seems like a reasonable precaution to take. Likewise, if you believe you are in the early stages of frozen shoulder, take the ‘use it or lose it’ approach. Use as much of your available range as possible without excessive pain (see above, discomfort is ok, pain is not!). Ask your osteopath for some exercises that can help maintain the range as much as possible. If the pain levels are such that you can’t move it without undue discomfort, imagine moving it around as you would do normally. While this sound like wishful thinking, it is actually sound advice based on what we know about movement. Again, my patients will have heard this many times before, but a large part of both movement in general and movement disorders is neurological. A lot of the time, the ‘issue is not in the tissue’, but in the command and control. When we lose RoM, it is both a physical and neurological loss; so if you can’t work on the physical movement itself, focus on the neurological component. Numerous experiments have shown that we can improve physical skills, including flexibility, by imagining ourselves practising that skill or stretch. This is because thinking about doing something, and actually doing it, are very similar neurologically speaking. If you look at brain scans of people performing a particular movement or activity, and those just imagining it, you won’t see much difference (Assuming, of course, you can read the scans at all!). This might also help to explain why a period of immobilisation can predispose toward FFS, as can sedentary lifestyles – your nervous system and muscles become habituated to a limited range of movement. Recommended reading: Frozen shoulder: a consensus definition. Zuckerman JD, Rokito A, J Shoulder Elbow Surg. 2011 Mar; 20(2):322-5. [i] Wong CK1, Levine WN2, Deo K3, Kesting RS3, Mercer EA3, Schram GA3, Strang BL3 “Natural history of frozen shoulder: fact or fiction? A systematic review.” Physiotherapy. 2017 Mar;103(1):40-47. [ii] Vermeulen HM, Stokdijk M, Eilers PH. “Measurement of three dimensional shoulder movement patterns with an electromagnetic tracking device in patients with a frozen shoulder” Ann Rheum Dis. 2002;61:115–120. [iii] Favejee MM, Huisstede BM, Koes BW. “Frozen shoulder: the effectiveness of conservative and surgical interventions – systematic review” Br J Sports Med. 2011;45:49–56. [iv] Jain TK, Sharma NK. The effectiveness of physiotherapeutic interventions in treatment of frozen shoulder/adhesive capsulitis: a systematic review. J Back Musculoskelet Rehabil. 2014;27:247–273. [v] Ogilvie-Harris DJ, Biggs DJ, Fitsialos DP, MacKay M. The resistant frozen shoulder: manipulation versus arthroscopic release. Clin Orthop. 1995;319:238–248 Leave a Reply. |
AuthorsDrs. Edmund Bruce-Gardner and Soraya Burrows are osteopaths Categories
All
|
|
Osteopathy at Moreland Road Clinic
High quality & personalised service from experienced professionals. A safe, effective & collaborative approach to patient care. All osteopaths undertake a 4-5 year university degree and are licensed and registered healthcare pracitioners. |
Find Us
Moreland Road Clinic 85 Moreland Road Coburg VIC 3058 P (03) 9384 0812 F (03) 9086 4194 osteopathy@morelandroadclinic.com.au |
Popular Blog Posts
|
|
|
Osteopathy at Moreland Road Clinic is on Moreland Road, near the corner of Nicholson Street/Holmes Street, on the border of Coburg, Brunswick & Thornbury.
This makes Osteopathy at Moreland Road Clinic the ideal location for people in the inner north and outer northern suburbs of Melbourne, including: Coburg, Coburg North, Coburg East, Brunswick, Brunswick East, Brunswick West, Fawkner, Oak Park, Glenroy, Preston, Pascoe Vale, Pascoe Vale South, Gowanbrae, Hadfield, Essendon, Moonee Ponds, Thornbury and Reservoir. |
6/3/2018
0 Comments