MRCO BLOG
Medical Musings, Health Hypotheses & Therapeutic Thoughts
 Low back pain (LBP) can be due to any one of a number of different causes. Obviously, stressing/straining the local muscles, ligaments, joints etc. will cause pain and discomfort, but as with the shoulder, other structures in the body are also capable of ‘throwing’ pain to a distant location. The kidneys, small intestine, colon/rectum, stomach, pancreas, spleen, gallbladder etc. are all known to cause low back pain. Surprising few of the female readers of this blog, the ovaries and uterus (womb) are also more than capable of causing low back discomfort (especially at ‘that time of the month’ or during pregnancy); as are problems with the blood vessels, heart, various types of infection, cancers, and hormone disorders. Because of this, it is always important to have your back pain screened by an appropriately-trained healthcare professional, especially if you have noticed other changes before or after the onset of the pain. For the purposes of this blog, we will ignore all of the slightly more esoteric factors, and instead focus on non-specific (or mechanical) low back pain. As mentioned above, this is usually due to irritation of the moving parts of the spinal column, namely muscles, tendons, ligaments, vertebral bodies, intervertebral discs (the ‘shock absorbers’ between the vertebrae), and facet joints (the joints between one level of the spine and another). Most mechanical low back pain resolves on its own, most often within 2-4 weeks. However, that can feel like a long time when you are in pain! So, what can you do to help speed that process up? Manual therapy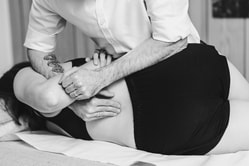 Such as osteopathy can help to alleviate the symptoms of low back pain. This is largely done by influencing the central nervous system (your brain and spinal cord) rather than directly affecting the areas being worked on, but mobilising restricted joints, stretching out tight muscles, and improving blood flow to the affected areas, can all help to mitigate the impact of mechanical LBP. Movement It might feel like the last thing we want to do when we are in pain, especially when we have not identified which movements trigger pain, but movement is medicine, as many of my patients have heard time and again. The key here is pain-free movement. If it hurts to bend backwards too far, then only go as far as you can without causing yourself undue discomfort! You should nearly always be able to find some positions or movements that do not aggravate your pain too much, even if it is a bit uncomfortable to do so. The problem with inactivity is that it impairs the blood flow to and from the affected areas, slowing the healing process. The spinal column has up to eight (depending on definition) pump systems that help to support its health, which rely on normal physiological (to do with normal function of living organisms and their systems) movement to drive them. This is, in part, what osteopathic treatment does: to mimic these normal movements and restore some of these pumps. It also helps to ‘show’ the body that nothing catastrophic will happen if it allows a little bit more movement through the area (the influencing of the central nervous system we were talking about earlier), thus promoting further relaxation and decrease of nociception (the nervous system’s response to harmful/potentially harmful stimuli, i.e. the first part of feeling pain). Having said all of that, exercising when your back is in full spasm (i.e. just after the injury) may be counterproductive, if the body feels like it is under attack, it will try to protect itself (largely by tightening up the muscles further). Make sure you listen to your body, and don’t perform any movements or activities that actually hurt (some discomfort is normal, and to be expected). If you cannot move at all without pain, then consider: Rest This does not mean weeks of bed-rest, as may have been recommended a few decades ago. That is pretty much the worst thing you can do (see above!). Rest for no more than 48 hours following the injury (or the first time you notice the pain, if there is no traumatic cause). Getting up and at ‘em (with slowly increasing activity levels) once you notice that initial acute phase subsiding will ease pain and stiffness, and speed up the healing process (again, see above!). Heat & Cold As a general rule of thumb, cold is good for decreasing inflammation (the first part of the body’s response to injury, and the start – theoretically, at least – of the healing process), so is advised in the first 72 hours or so after injury. Cold also ‘confuses’ the nervous system – it can’t work out whether to focus on the cold or the pain signals, an effect know as pain-gating. It is the same mechanism when a parent rubs on the banged elbow or barked knee of a child: the pressure of the rubbing decreases the amount of attention the brain pays to the pain stimulus. You don’t need an ice-pack, specifically, just wrap a tea-towel or similar around a bag of frozen peas or other vegetables (never put anything too cold into direct contact with the skin). Heat is very good for helping tight and sore muscles relax, and increasing the blood flow to an area. How good does a nice hot bath (or shower) feel after a long day of working hard?! However, both have their caveats: Heat will aggravate any inflammation present, and part of the inflammatory process is to increase fluid in the area (swelling), so the last thing you need is more blood flow to the injured part. Cold also has the potential to cause muscles to contract to protect themselves and keep warm. So, the golden rule is: if you put on ice/heat and it makes it feel worse, then stop! Ask your osteopath whether heat or ice would be more appropriate given the nature of your injury. Pharmacological (drug) management Over-the-counter (OTC) medications, such as acetaminophen (Panadol) or non-steroidal anti-inflammatories (NSAIDs) such as ibuprofen (e.g. Neurofen) or sodium diclofenac (Voltaren), may help with your back pain. We know that these drugs are not very good at helping with chronic back pain, and are not a good long-term management strategy, but in acute cases they may help to ease a bit of discomfort, which then allows you to move a little more easily, which speeds up the healing process (as noted above, the protective spasm or muscle guarding that normally takes place in response to an injury actually restricts blood-flow to an area, slowing down the healing process). Please note: I am not qualified to give pharmaceutical advise. Always read the label, and consult your doctor or pharmacist regarding the suitability of any given medication for you and your condition. Stretching and Exercise This is such a big topic that I will only devote a few words to it here, saving the rest for another blog post. Maintaining mobility and flexibility is one of the biggest things you can do to help prevent injury, but in the instance that it’s a little bit late (after all, you’re reading this looking for tips as to how to manage your existing low back pain), there is also a lot you can do now. In general, the basic tenet is that movement is medicine, and both stretching to relax muscles and general mobilisation (taking the joints and muscles through their normal range repeatedly) can help significantly with your symptoms. For further details, please see here. Leave a Reply. |
AuthorsDrs. Edmund Bruce-Gardner and Soraya Burrows are osteopaths Categories
All
|
|
Osteopathy at Moreland Road Clinic
High quality & personalised service from experienced professionals. A safe, effective & collaborative approach to patient care. All osteopaths undertake a 4-5 year university degree and are licensed and registered healthcare pracitioners. |
Find Us
Moreland Road Clinic 85 Moreland Road Coburg VIC 3058 P (03) 9384 0812 F (03) 9086 4194 osteopathy@morelandroadclinic.com.au |
Popular Blog Posts
|
|
|
Osteopathy at Moreland Road Clinic is on Moreland Road, near the corner of Nicholson Street/Holmes Street, on the border of Coburg, Brunswick & Thornbury.
This makes Osteopathy at Moreland Road Clinic the ideal location for people in the inner north and outer northern suburbs of Melbourne, including: Coburg, Coburg North, Coburg East, Brunswick, Brunswick East, Brunswick West, Fawkner, Oak Park, Glenroy, Preston, Pascoe Vale, Pascoe Vale South, Gowanbrae, Hadfield, Essendon, Moonee Ponds, Thornbury and Reservoir. |
8/10/2018
0 Comments